Life in the 21st century is full of electronic devices and apps purported to make life easier. Many of us can binge watch movies, videos and news on our phones. There are wireless headphones, electric bicycles, self-operating vacuum cleaners, wine in boxes with taps—and so much more.
This life is, however, not without challenges.
In the event that you or yours ends up in the hospital, the stay could be complicated by an unplanned, unwanted and potentially lethal infection.
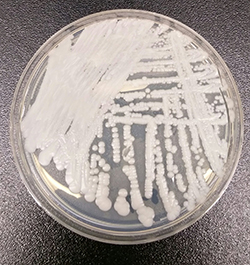
No thanks to the yeast, Candida auris.
As Matt Richtel and Andrew Jacobs wrote in The New York Times recently, in the article “A Mysterious Infection, Spanning the Globe in a Climate of Secrecy”,
“The rise of Candida auris embodies a serious and growing public health threat: drug-resistant germs.”
In their April 6 article, Richtel and Jacobs bring to our attention a microbial infection that killed a patient and left the patient’s hospital room contaminated. The responsible microbe was C. auris, an emerging fungal pathogen. Hospitals have not been successful in getting rid of this fungus, and it has shown the ability to resist first-, second- and even third-line antifungal drugs.
Candida Auris: Unstoppable?
C. auris was originally identified in greenish-yellow drainage from the ear canal of a woman in Japan in 2009 (CDC). (Auris is Latin for ear.) However, the Centers for Disease Control (CDC) states that the earliest known strain of C. auris dates to South Korea and 1996.
C. auris infection has been identified in many countries including South Africa, Venezuela, India, China, Russia and Australia.
In addition to the ear canal, C. auris can infect the urinary tract, wound sites, in-dwelling catheters and blood lines. When immunocompromised persons are exposed to C. auris, the risk of infection is quite high.
Fisher et al., reported in Science, May 18, 2018 that,
“Worldwide emergence of resistance to antifungal drugs challenges human health and food security”
providing a broader (and more depressing) angle on this fungal infection. Candida auris might be our canary in the coal mine, the harbinger of what is to come.
Stopping the Unstoppable
There is no question that C. auris is a deadly and very serious pathogen. But there are means by which to approach this fungus that can improve the chances of overtaking it.
The April 6 New York Times story details how an infectious disease specialist responded to an urgent need to decontaminate a British medical center where C. auris had “taken root”. The hospital had not been successful in clearing the pathogen.
Using a special aerosol device, the disease specialist had the room sprayed with hydrogen peroxide (H2O2) for an entire week. After the decontamination, they checked the room again. There was a single surviving organism: C. auris.
The CDC has a web site with recommendations on how to decontaminate successfully when C. auris is present. H2O2 was not the only recommended antimicrobial cleaning agent. Of six agents examined from the list, only one contained peroxide; five others were bleach-containing compounds.
The CDC’s recommended decontamination protocol for C. auris is the same as that for Clostridium difficle spores. C. difficle is a bacterium that can wreck havoc with the hospitalized. C. difficile produces spores which are notoriously difficult to kill. The CDC recommends “LIST K: EPA’s Registered Antimicrobial Products Effective against Clostridium difficile Spores” for use against C. auris.
Know Your Pathogen
In 2017 Lockhart et al. published a paper in the Journal of Clinical Microbiology, “Thinking beyond the common Candida species: Need for speciation of Candida due to the emergence of multidrug resistant Candida auris”. Shawn Lockhart, the lead author, is Director of the Fungal Reference Laboratory at the CDC.
In the paper Dr. Lockhart noted the importance of speciation of invasive Candida isolates, saying that
“each species has specific antifungal drug susceptibility patterns that can inform treatment decisions”.
Lockhart says it’s common for invasive Candida infections to be treated without species conformation, a practice he says is
“similar to treating a Gram-negative infection without knowing whether the causative bacterium is Escherichia coli, Pseudomonas aeruginosa or a rare pathogen.”
(Those familiar with microbial pathogens know that E. coli is no less pathogenic but usually much more susceptible to antimicrobials than the terrifically hard-to-treat P. aeruginosa. )
Lockhart also pointed out that C. auris requires contact precautions and infection control measures not recommended for most other Candida species, essential in order to control and prevent the spread of this yeast—another reason why it is important to identify Candida isolates to the species level.
Species identification of Candida isolates can be problematic. Lockhart noted that U.S. hospital laboratories often don’t have the ability or equipment for this level of fungal identification. Hospitals often identify Candida sp. isolates using commercial yeast identification systems (see Lockhart et al. for a list) that are not capable of this level of identification.
Worse yet, some commercial systems, instead of giving a “no identification” warning, often misidentify C. auris as a different Candida species.
The CDC can help with identification of Candida isolates and antifungal drug susceptibility testing.
Secrecy is Another Issue
Richtel and Jacobs, in The New York Times article, reveal the secrecy with which hospitals, even in the U.S., treat Candida auris infections. Could sending a sample to the CDC for species identification result in identification of the hospital the organism came from? A potential “outing” of a hospital as one contaminated with C. auris could be really bad for business.
But think of the enormous importance to patients of knowing exactly what they are infected with. This information affects their drug therapy, who comes and goes from their room, and the level of care facility they are in, not to mention how the room and equipment around them is cleaned.
What if clinicians were treating patients with antifungals after speciation of the Candida strain, so that they were using the correct anti-fungal agent? Could the incidence of C. auris infections be cut simply by using disinfecting agents that were proven to work?
Emerging Pathogens: A Broader View
Fisher et al. (Science, May 2018) promote the need for new solutions as well, such as the need to improve stewardship of existing antifungal chemicals, promote the discovery of new antifungals and leverage emerging technologies in order to find new, alternative solutions to fungal pathogens.
Could wine in a box, crowd sourcing and binge watching are somehow part of the solution? What if there was an app that identified C. auris by phone? The sooner we know the pathogen, the more quickly it can be stopped.
In the meantime we need to identify, treat and disinfect emerging infections like C. auris, using the best information available, without delay.
Kari Kenefick
Latest posts by Kari Kenefick (see all)
- Base Editing Brilliance: David Liu’s Breakthrough Prize and Its Impact - May 28, 2025
- Neurons’ Role in FBP2 Regulation - October 24, 2024
- Fluorescent Ligands in Biological Research: Where We’ve Been, Where We’re Headed - June 27, 2024
