The term ICOS —inducible T cell co-stimulators— has been prominent in my work as a science writer at Promega, recently. Here is a brief look at ICOS, how it works, and how it can be used in therapeutics research and development.
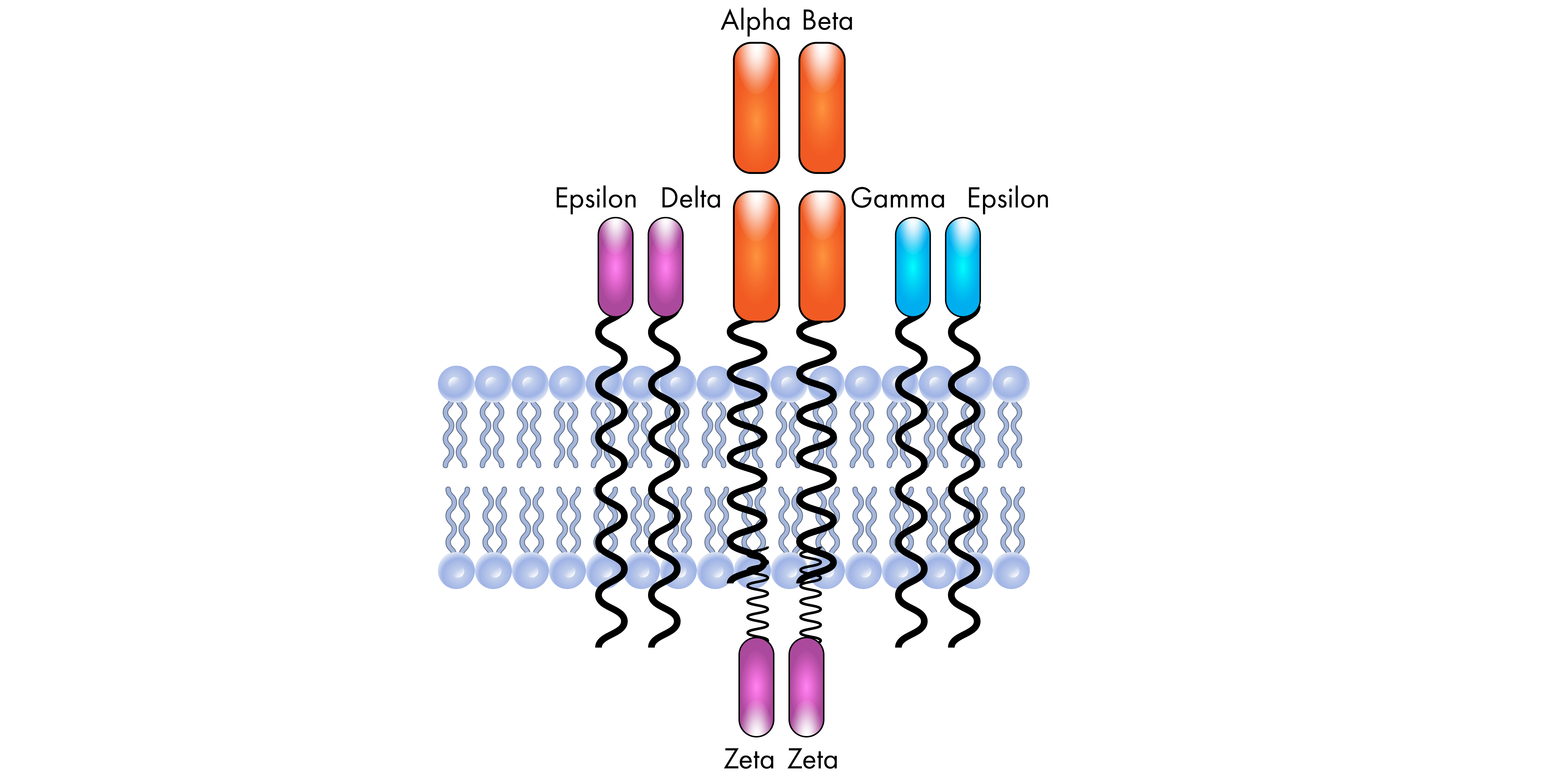
T cells do amazing things, like driving or blocking production of B cells and their related antibodies and antibody maturation, and they are the primary drivers of innate immunity. T cells have a variety of surface molecules, the primary and omnipresent T cell receptor (TCR), as well as CD3.
In the past 15 years or so, researchers have identified other, inducible receptors on T cells. These receptors appear when T cells are stimulated, enabling interactions with other cell types. The following information is summarized from a Frontiers in Immunology review by Wikenheiser et al.
What is ICOS (inducible T cell co-stimulators)?
ICOS or ‘inducible T cell co-stimulators’ are T cell surface molecules that appear only after the T cell receptor (TCR) is bound or after CD3 cross-linking. They are not constitutively expressed on the T cell surface.
ICOS is involved in activation and stimulation of T cells, in collaboration with other surface molecules like the T cell receptor (TCR) and CD3. Once attached to the ICOS ligand (ICOSL), ICOS sends signals to the nucleus through a cascade of molecules including p85alpha, p110delta and OPN (osteopontin).
Need a reminder on T cell and B Cell function? This immunology primer might help.
Ten Things to Know about ICOS
1) ICOS plays an essential role in development of adaptive immunity. It was identified first in humans, then in mice.
2) ICOS is necessary for development of memory T cells. Human ICOS deficiency is associated with fewer circulating CD4+ memory T cells relative to healthy controls. Data suggest ICOS promotes formation and maintenance of a stable population of CD4+ memory T cells, and in certain cases may influence their re-activation.
3) ICOS promotes induction, maintainance and follicular homing of T follicular helper cells.
4) ICOS is a member of the immunoglobulin (Ig) family of receptors.
5) ICOS structure is similar to CD28, but their roles are exclusive. While CD28 and CTLA-4 interact with corresponding receptors CD80 and CD86, ICOS interacts exclusively with ICOSL.
6) ICOSL is found mainly on mature antigen-presenting cells. It’s expression is downregulated following binding to ICOS.
7) ICOS deficient T cells have a proliferation defect in vitro, and Icos-/- mice, after antigen treatment, have smaller lymph nodes than normal mice treated with the same antigen.
8) In response to various infective agents, viral, bacterial or parasitic, ICOS regulates T helper cell subsets, by either promoting or inhibiting Th1 and Th2 immune responses. In M. tuberculosis-infected, ICOS-deficient mice, the Th1 response was strong, while Treg T cell populations were greatly reduced. Furthermore, M. tuberculosis infection was controlled in the spleens of ICOS-deficient mice, eventually, but not in their lungs.
9) Development of Th2 immunity appears to be more reliant on ICOS signaling than is Th1 immunity. In several infection models, disruption of ICOS signaling led to decreased IL-4 production, as well as reduced expansion of CD4+ T cells, required for Th2 immunity. Similar to infection models that induce a Th1 response, the absence of ICOS signaling did not completely suppress the development of Th2 immunity, but rather delayed it.
10) While early observations connected ICOS co-stimulation with Ab production, these authors found conflicting results on the role of ICOS in promoting Ab responses. What is certain is that ICOS is a critical component in the production of isotype-switched IgGs, particularly affinity-matured Abs.
ICOS as a Target for Therapeutics
Data cited by Wikenheiser et al. suggest that ICOS plays a role in promoting tissue damage seen in systemic lupus erythematosis (SLE) disease progression in mice and humans. Graft versus host disease (GVHD) and airway hyperreactivity (AHR), an indicator of asthma, can both be promoted by ICOS, and therapeutic antibodies designed to block ICOS, have shown promise, but also serious and unintended side effects.
ICOS and ICOSL blocking or promoting therapies are poised to provide relief to suffers of autoimmune and other disease syndromes such as SLE and GVHD.
Yet there are unanswered questions and room for discovery in the roles of ICOS and ICOSL in T cell development.
Reference
Wikenheiser, D.J. and Stumhofer, J.S. (2016) ICOS Co-Stimulation: Friend or Foe? Front. Immunol. 7:304.
Related Posts
Kari Kenefick
Latest posts by Kari Kenefick (see all)
- What Drives Muscle Fiber Shifts in Obesity and Type ll Diabetes? - October 9, 2025
- How Thalidomide and Molecular Glues Are Redefining Drug Discovery - August 21, 2025
- ATP-Powered Proteins Beyond Kinases – and Why Helicases Are Stealing the Spotlight - August 7, 2025
